Anatomy of Parotid Gland. The paired parotid gland is the largest of the three pairs of salivary glands (parotid, submandibular, and sublingual). It is an irregular, lobulated, yellowish mass, lying largely below the external ear canal. Its shape is similar to a inverted pyramid. Each gland weighs about 25 g. It is located in a depression called retromandibular fossa (parotid bed) that is inferior to the auricle and posterior to the ramus of the mandible.
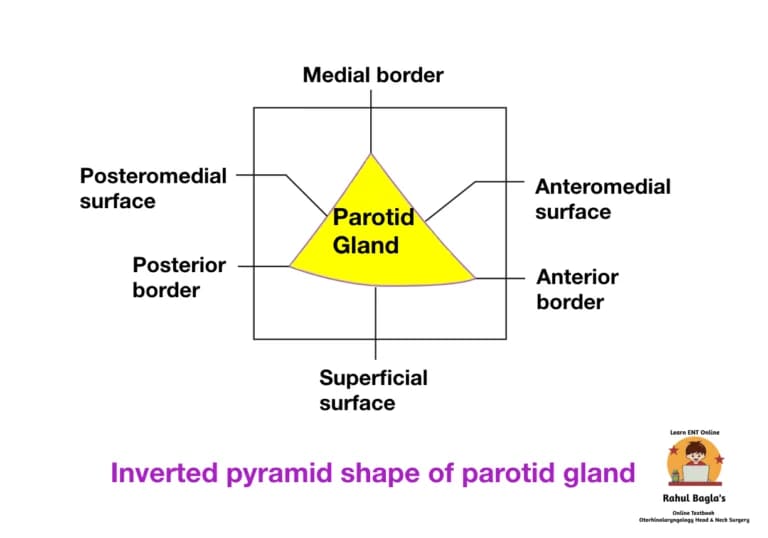
Boundaries of the Retromandibular fossa (parotid bed).
- Superiorly: External auditory canal and posterior part of temporomandibular joint.
- Medially: Styloid process.
- Anteriorly: Posterior border of the ramus of mandible
- Posteriorly: Mastoid process.
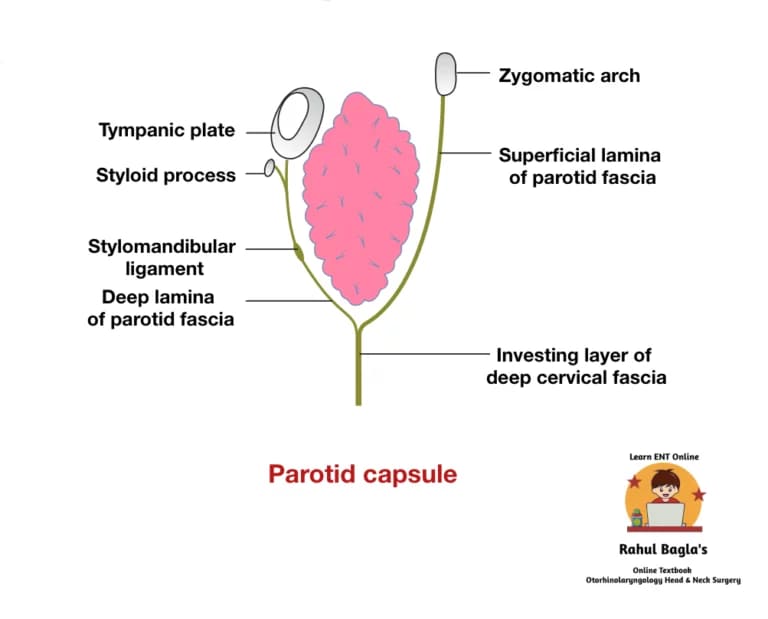
Parotid capsule (parotid sheath). Parotid capsule is a strong tough fibrous capsule formed by investing layer of deep cervical fascia which encases the parotid gland. Due to strong nature of the capsule any stretching or tension of the capsule due to any inflammation causes severe excruciating pain. Pain is also due to stimulation of the greater auricular nerve.
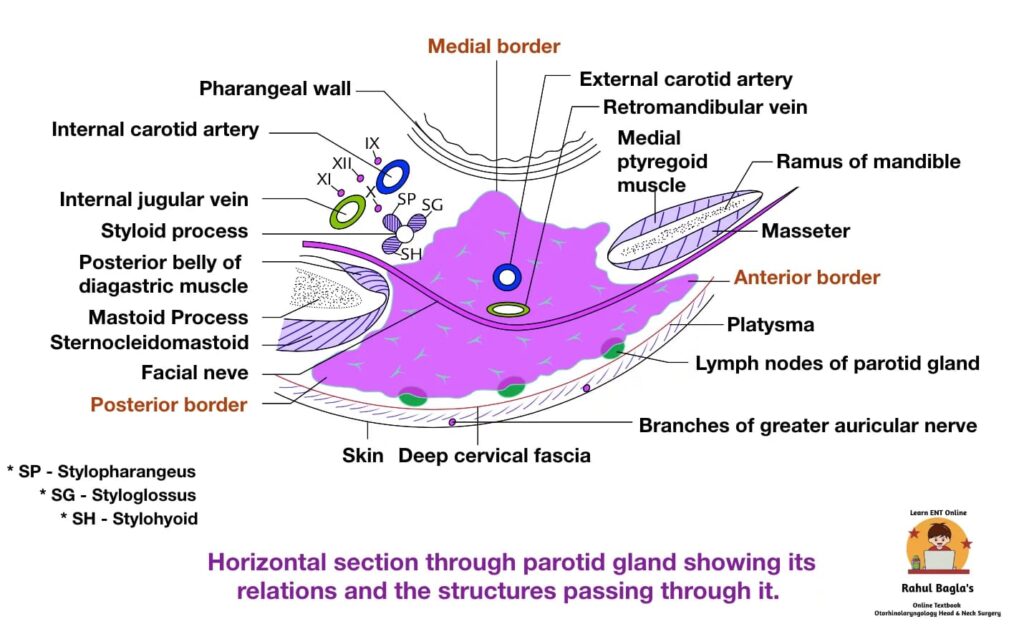
Muscles related to parotid bed.
- Ramus of the mandible is covered by two muscles: masseter laterally and the medial pterygoid medially.
- Mastoid process is covered by two muscles: sternocleidomastoid laterally and posterior belly of digastric muscle medially.
- Styloid process is enveloped by three muscles: styloglossus, stylopharyngeus, and stylohyoid.
 Structures present within the parotid gland. Three main structures either in part or in whole traverse the gland and branch within it. From superficial to deep these are:
Structures present within the parotid gland. Three main structures either in part or in whole traverse the gland and branch within it. From superficial to deep these are: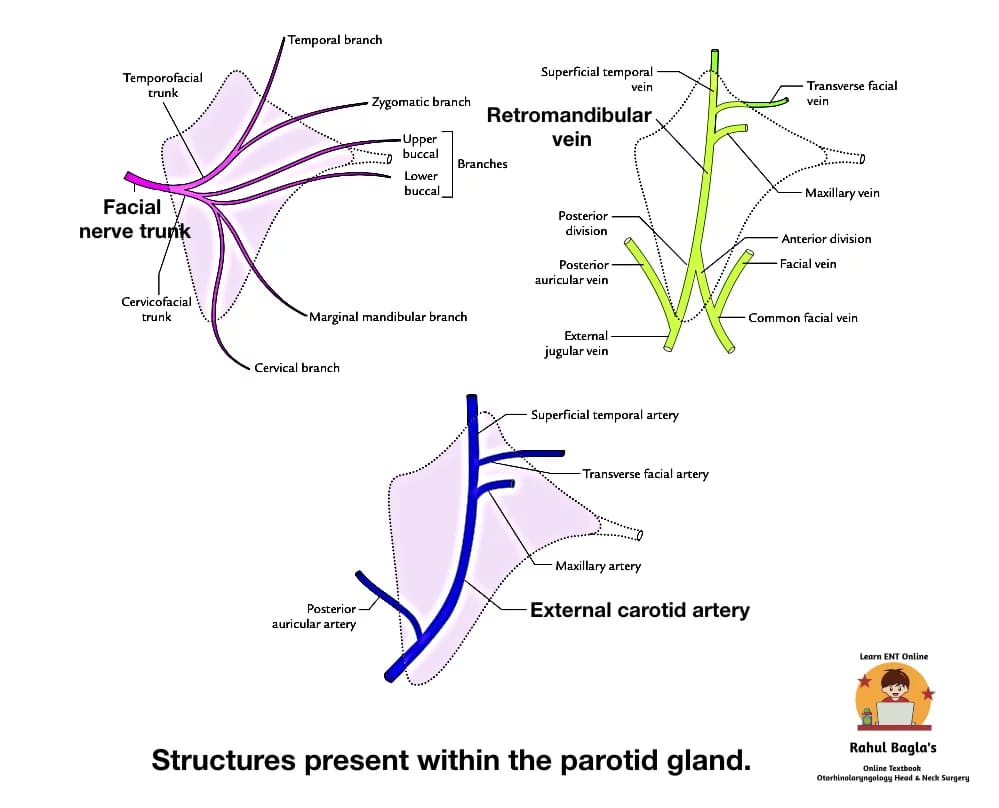
- Facial nerve.
- Retromandibular vein.
- External carotid artery.
Facial nerve is most superficial and enters the parotid gland high up on its posteromedial surface. Within the substance it divides into in to superior (temporo-facial) and inferior (cervico-facial) trunks. It further divides horizontally into terminal branches within the gland forming parotid plexus (pes anserinus). It leaves the gland through its anteromedial surface and appear on the face to supply the muscles of facial expression.
Retromandibular vein is superficial to the external carotid artery. It is formed by the union of the superficial temporal and maxillary veins. It divides into an anterior branch, which passes forwards to join the facial vein, and a posterior branch, which joins the posterior auricular vein to form the external jugular vein.
External carotid artery enters the lower part of the posteromedial surface and divides into the maxillary artery, which emerges from the anteromedial surface, and the superficial temporal artery, which gives off its transverse facial branch in the gland and ascends to leave its upper limit. The transverse facial artery, branch of superficial temporal artery emerges through the anterior border of the gland. The posterior auricular artery may also branch from the external carotid artery within the gland, leaving by its posteromedial surface.
Division of superficial and deep lobe. The parotid gland is divided into large superficial and small deep parts, connected by the H-shaped isthmus. Facial nerve branches passes through the isthmus. This plane between the superficial and deep lobes is called as “Patey’s faciovenous plane“. It helps the surgeons to remove the parotid tumor without damaging the nerve.
Course of Parotid duct (Stenson’s duct). It is about 5 cm long. It emerges from the middle of the anterior border of the gland. It runs forward over the masseter between the upper and lower buccal branches of the facial nerve. Then it turns 90° piercing the buccinator muscle, runs forward for 1 cm and then, the duct turns medially and opens into the vestibule of mouth opposite the crown of upper second molar teeth.
Anatomy of Parotid Gland Anatomy of Parotid Gland Anatomy of Parotid Gland Anatomy of Parotid Gland Anatomy of Parotid Gland Anatomy of Parotid Gland Anatomy of Parotid Gland
Nerve supply.
The parotid gland is supplied by the parasympathetic, sympathetic, and sensory fibres:
1. Parasympathetic (secretomotor) supply: It is provided through auriculotemporal nerve. The preganglionic fibres arise from the inferior salivatory nucleus in the medulla and pass successively through glossopharyngeal nerve, tympanic branch of glossopharyngeal (Jacobson’s nerve), tympanic plexus and lesser petrosal nerve to relay into otic ganglion. Postganglionic fibres arise from the cells of the ganglion and pass through the auriculotemporal nerve to supply the parotid gland. The stimulation of parasympathetic supply produces watery secretion.
2. Sympathetic supply: It is derived from sympathetic plexus around external carotid artery formed by postganglionic fibres derived from superior cervical sympathetic ganglion. The sympathetic fibres are vasomotor and their stimulation produces thick sticky secretion.
3. Sensory supply: It is derived from:
- Auriculotemporal nerve.
- Great auricular nerve (C2 and C3). The C2 fibres are sensory to the parotid fascia.
Blood supply.
- Arterial supply – External carotid and superficial temporal arteries.
- Venous drainage – Retromandibular and external jugular veins.
Lymphatic drainage.
The lymphatics from the parotid gland drain into the superficial and deep parotid lymph nodes, which in turn drain into deep cervical lymph nodes.
Parotid Gland – Anatomy Function Innervation Parotid Gland – Anatomy Function Innervation Parotid Gland – Anatomy Function Innervation Parotid Gland – Anatomy Function Innervation
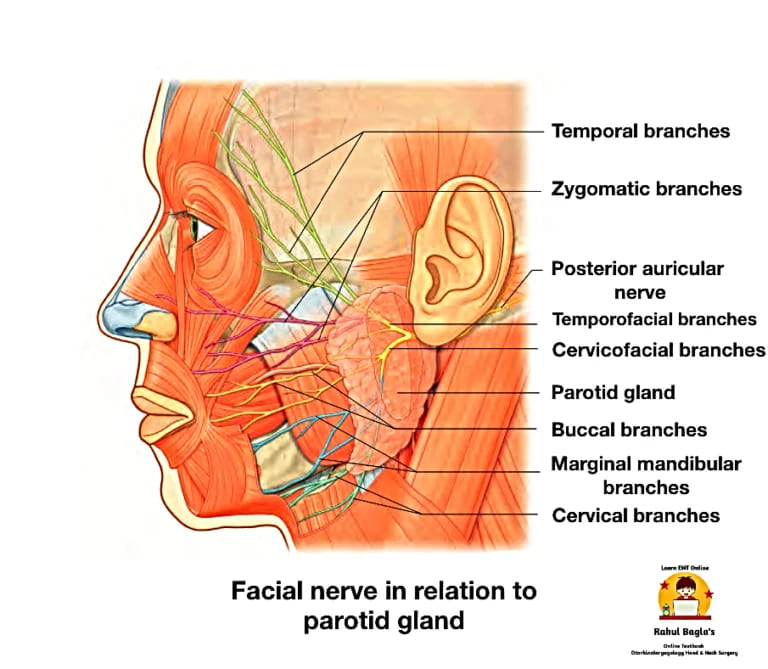
Facial nerve in relation to parotid gland.
After emerging from the stylomastoid foramen, it curves forwards around the lateral aspect of the root of the styloid process and enters the posteromedial aspect of the parotid gland on the superficial plane.
In the gland, it runs superficial to the retromandibular vein for about 1 cm and then divides into two trunks:
- The temporofacial trunk runs upwards and subdivides into temporal and zygomatic terminal branches
- The cervicofacial trunk passes downwards and forwards, and divides into buccal, marginal mandibular, and cervical terminal branches.
Terminal branches: These are five in number, viz.:
- Temporal branch—run upwards and cross the zygomatic arch.
- Zygomatic branches—run below and parallel to the zygomatic arch.
- Buccal branches—are two in number. The upper buccal nerve runs above the parotid duct and the lower buccal nerve runs below the duct.
- Marginal mandibular (also called mandibular) branch – runs forwards below the angle of the mandible, deep to the platysma. It then crosses the body of the mandible to supply the muscles of the lower lip and chin.
- Cervical branch—runs downwards and forwards to reach the front of the neck, to supply the platysma.
Comparison of the Three Major Salivary Glands

———— End of the chapter ————
Download full PDF Link:
Anatomy of Parotid Gland Best Lecture Notes Dr Rahul Bagla ENT Textbook
Reference Textbooks.
- Scott-Brown, Textbook of Otorhinolaryngology-Head and Neck Surgery.
- Cummings, Otolaryngology-Head and Neck Surgery.
- Stell and Maran’s, Textbook of Head and Neck Surgery and Oncology.
- Ballenger’s, Otorhinolaryngology Head And Neck Surgery
- Susan Standring, Gray’s Anatomy.
- Frank H. Netter, Atlas of Human Anatomy.
- B.D. Chaurasiya, Human Anatomy.
- P L Dhingra, Textbook of Diseases of Ear, Nose and Throat.
- Hazarika P, Textbook of Ear Nose Throat And Head Neck Surgery Clinical Practical.
- Mohan Bansal, Textbook of Diseases of Ear, Nose and Throat Head and Neck Surgery.
- Hans Behrbohm, Textbook of Ear, Nose, and Throat Diseases With Head and Neck Surgery.
- Logan Turner, Textbook of Diseases of The Nose, Throat and Ear Head And Neck Surgery.
- Arnold, U. Ganzer, Textbook of Otorhinolaryngology, Head and Neck Surgery.
- Ganong’s Review of Medical Physiology.
- Guyton & Hall Textbook of Medical Physiology.
Author:

Dr. Rahul Bagla
MBBS (MAMC, Delhi) MS ENT (UCMS, Delhi)
Fellow Rhinoplasty & Facial Plastic Surgery.
Renowned Teaching Faculty
Mail: msrahulbagla@gmail.com
India
———– Follow us on social media ————
- Follow our Facebook page: https://www.facebook.com/Dr.Rahul.Bagla.UCMS
- Follow our Instagram page: https://www.instagram.com/dr.rahulbagla/
- Subscribe to our Youtube channel: https://www.youtube.com/@Drrahulbagla
- Please read. Juvenile Angiofibroma. https://www.entlecture.com/juvenile-angiofibroma/
- Please read. Tumours of Hypopharynx . https://www.entlecture.com/tumours-of-the-hypopharynx/
- Please read. Anatomy of Oesophagus. https://www.entlecture.com/anatomy-of-oesophagus/
Keywords: Explore the detailed anatomy of the parotid gland, including its structure, ducts, blood supply, and innervation, along with clinical insights, Parotid Gland – Anatomy, Function, Innervation, Stenson’s duct, Parotid capsule, Parotid Bed, Salivary gland, Facial nerve, Parotid gland anatomy, Structure of the parotid gland, Parotid gland location, Functions of the parotid gland, Parotid gland ducts, Blood supply to the parotid gland, Parotid gland innervation, Detailed anatomy of the parotid gland and its ducts, What is the location and function of the parotid gland? Parotid gland anatomy explained for medical students, Blood supply and nerve innervation of the parotid gland, Salivary gland anatomy: Focus on the parotid gland, Role of the parotid gland in salivation, Common diseases related to the parotid gland anatomy, What is the parotid gland, and where is it located?, How does the parotid gland contribute to salivation? Understanding the anatomy of the parotid gland step by step, What are the ducts of the parotid gland and their functions? Common clinical conditions affecting the parotid gland, Parotid gland histology, Gross anatomy of salivary glands, Facial nerve relation to parotid gland, Parotid gland surgical anatomy, Anatomical landmarks near the parotid gland
