|
The following CBME core competencies are covered in this chapter.
|
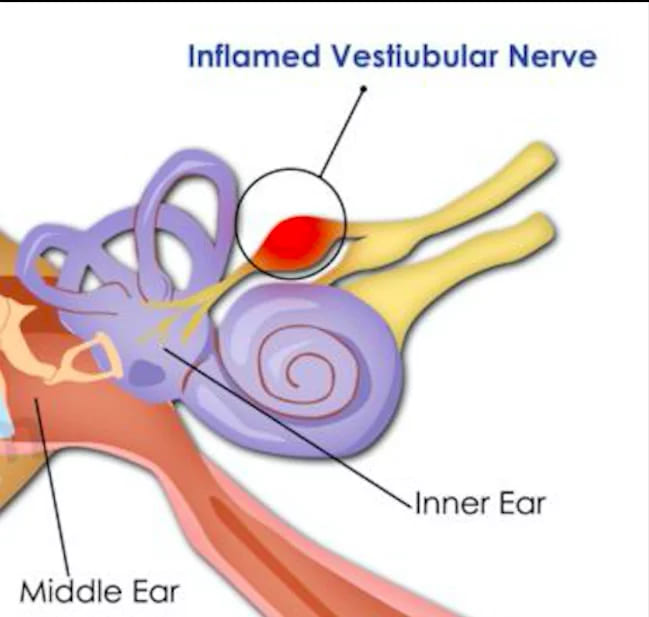
Vestibular Neuritis. It is also known as acute peripheral vestibular loss caused by selective inflammation (presumed to be of viral in origin) of the vestibular nerve (which is branch of the vestibulocochlear nerve). It is second most common cause of vertigo following BPPV.
The vestibular nerve innervates the vestibular system of the inner ear and maintains balance of the body, while the cochlear nerve travels to cochlea of the inner ear and it is responsible for sense of hearing.
It is characterized by acute onset of sustained severe vertigo associated with nausea, vomiting. There are no cochlear symptoms (hearing loss and tinnitus) or neurological symptoms. Disease is considered as a benign, self-limited, symptoms may last from a few days to 2 or 3 weeks and patient is usually bed bound during this phase. Although labyrinthitis is closely related but vestibular neuritis is differentiated by its auditory preserving function.
Aetiology. The exact cause remains obscure. The suggested causes are:
- Most commonly it is associated with preceding or accompanying viral infection. It is believed to occur due to the reactivation of a latent virus herpes simplex virus type 1 (HSV-1) in vestibular ganglion. Other viruses which can cause isolated peripheral vestibular dysfunction are rubella, cytomegalovirus, Epstein–Barr virus, adenovirus and influenza types A and B.
- Head trauma may cause acute vestibular loss.
- Vascular and immunological causes.
Clinical features and diagnosis:
- The acute phase lasts 48 to 72 hours. Spontaneous nystagmus is commonly seen but usually subsides within first 48-72 hours. Horizontal-torsional spontaneous type nystagmus is present, beating towards unaffected side.
- Head thrust test. If corrective saccades are present, the test is considered positive on the same side.
- Gait test and Unterberger test show deviation to the side of the lesion
- Romberg test shows marked increase of sway.
- Caloric testis gold standard for diagnosis. There is reduced or absent response on the affected side.
- Mostly vestibular neuritis is unilateral, bilateral involvement are also reported. The rotatory chair test (used in combination with VNG or ENG) is gold standard for diagnosis of bilateral vestibular loss.
Management. Acute attack management is similar to that in Meniere’s disease.
- Reassurance.
- Antiemetics: antiemetics are vestibular sedatives. Should be used only during the acute stage since long-term use prevents vestibular compensation.
- Antihistamines, anticholinergic agents and antidopaminergic agents are the most commonly used drugs.
- Fluid replacement may be necessary in particularly severe cases.
Vestibular rehabilitation is a safe and effective treatment for patients who do not recover fully within few weeks. It consists of the Cawthorne–Cooksey exercises.
———— End of the chapter ————
Download full PDF Link:
Vestibular Neuritis Best Lecture Notes Dr Rahul Bagla ENT Textbook
Reference Textbooks.
- Scott-Brown, Textbook of Otorhinolaryngology-Head and Neck Surgery.
- Glasscock-Shambaugh, Textbook of Surgery of the Ear.
- P L Dhingra, Textbook of Diseases of Ear, Nose and Throat.
- Hazarika P, Textbook of Ear Nose Throat And Head Neck Surgery Clinical Practical.
- Mohan Bansal, Textbook of Diseases of Ear, Nose and Throat Head and Neck Surgery
- Hans Behrbohm, Textbook of Ear, Nose, and Throat Diseases With Head and Neck Surgery.
- Salah Mansour, Middle Ear Diseases – Advances in Diagnosis and Management.
- Logan Turner, Textbook of Diseases of The Nose, Throat and Ear Head And Neck Surgery.
- Rob and smith, Textbook of Operative surgery.
- Anirban Biswas, Textbook of Clinical Audio-vestibulometry.
- Arnold, U. Ganzer, Textbook of Otorhinolaryngology, Head and Neck Surgery.
- Gordon B. Hughes, Myles L. Pensak, H. B. Broidy. Textbook of Clinical Otology.
- Mario Sanna. Textbook of Color Atlas of Endo-Otoscopy Examination–Diagnosis–Treatment.
Author:

Dr. Rahul Bagla
MBBS (MAMC, Delhi) MS ENT (UCMS, Delhi)
Fellow Rhinoplasty & Facial Plastic Surgery.
Renowned Teaching Faculty
Mail: msrahulbagla@gmail.com
India
———– Follow us on social media ————
- Follow our Facebook page: https://www.facebook.com/Dr.Rahul.Bagla.UCMS
- Follow our Instagram page: https://www.instagram.com/dr.rahulbagla/
- Subscribe to our Youtube channel: https://www.youtube.com/@Drrahulbagla
- Please read. Anatomy of External Ear. https://www.entlecture.com/anatomy-of-ear/
- Please read. Anatomy of Temporal Bone. https://www.entlecture.com/anatomy-of-temporal-bone/
- Please read. Stenger’s, Chimani Moos, Teal test. https://www.entlecture.com/special-tuning-fork-tests/
Keywords: Vestibular neuritis treatment guidelines, Comprehensive Guide to Vestibular Neuritis Treatment Protocols, Vestibular neuritis recovery exercises, Effective Recovery Exercises for Vestibular Neuritis Patients, Vestibular neuritis diet recommendations, Dietary Recommendations to Support Vestibular Neuritis Recovery, Vestibular neuritis alternative therapies, Exploring Alternative Therapies for Vestibular Neuritis Management, Vestibular neuritis in elderly patients, Understanding Vestibular Neuritis in Elderly Patients: Symptoms and Care, Vestibular neuritis vs. labyrinthitis differences, Vestibular Neuritis vs. Labyrinthitis: Key Differences Explained, Vestibular neuritis case studies, Case Studies Highlighting Vestibular Neuritis Diagnosis and Treatment, Vestibular neuritis and stress correlation, Investigating the Correlation Between Stress and Vestibular Neuritis, Vestibular neuritis long-term effects, Long-Term Effects of Vestibular Neuritis: What to Expect, Vestibular neuritis misdiagnosis cases, Common Misdiagnoses of Vestibular Neuritis and How to Avoid Them, Etiology, Clinical features, Diagnosis, Management, Vestibular rehab of, Vestibular Neuritis, Cawthorne–Cooksey exercises, Herpes simplex./p>
