Malignant (Necrotizing) Otitis Externa And Skull Base Osteomyelitis
Malignant (Necrotising) Otitis Externa
Introduction
Malignant otitis externa (MOE), also called necrotising otitis externa, is a severe, progressive infection of the external auditory canal (EAC) that can extend to involve the temporal bone and skull base. It is an ENT emergency because delayed diagnosis may lead to cranial nerve palsies, skull base osteomyelitis, and intracranial complications.
Key Concept (Spectrum of Disease):
- Stage 1 (Limited MOE): Infection confined to the EAC, bony-cartilaginous junction, and soft tissues.
- Stage 2 (Skull Base Osteomyelitis – SBO): Infection spreads beyond EAC to involve the temporal bone, petrous apex, jugular foramen, and lower cranial nerves.
Important note: “Malignant” is a misnomer (not cancer). “Necrotizing” is preferred. SBO is the complication, not a separate disease.
Definition
Malignant otitis externa (MOE), also called necrotizing otitis externa, is a severe progressive necrotizing infection of the external auditory canal, most commonly caused by Pseudomonas aeruginosa. Infection may spread to the temporal bone and jugular foramen, causing involvement of cranial nerves (especially VII, IX, X, XI, XII) and may lead to skull base osteomyelitis. Facial paralysis is a common complication.
Cardinal Sign (DO NOT MISS): In an elderly diabetic patient, severe otalgia with granulation tissue at the cartilaginous–bony junction of the external auditory canal is a cardinal sign of malignant otitis externa / skull base osteomyelitis and must not be underestimated.
Predisposing Factors / High-Risk Groups
- Elderly diabetic patients (90% of cases)
- Immunocompromised patients
- Patients on long-term steroid therapy
- Patients receiving chemotherapy
Pathogenesis
Normally, cerumen provides protection by maintaining an acidic pH, preventing maceration and excessive bacterial colonization. In diabetics, this protective mechanism is reduced, permitting bacterial overgrowth and increased susceptibility to tissue invasion.
Diabetic microangiopathy results in ischemic, nutritionally deficient and devitalized tissue. The infective process produces exotoxins and enzymes such as elastase, which can digest vessel walls. Impaired local and systemic immunity prevents control of infection, allowing progression from uncomplicated otitis externa to a fulminant invasive disease.
Pathways of Spread
The infection spreads from the EAC to adjacent skull base structures through natural anatomical pathways:
- Anterior spread: Infection spread to the skull base at the most vulnerable portion of the external canal, the osseocartilaginous junction, and proceed to infiltrate the parotid gland and facial nerve by way of the fissures of Santorini.
- Inferior spread: Traversing the tympanomastoid suture and fissures of Santorini provides access to the infratemporal fossa and jugular foramen, placing cranial nerves IX, X, and XI at risk for injury. Proximal injury results from involvement of the main trunk at the stylomastoid foramen via direct extension from the external auditory canal.
- Medial spread: Infection may spread to the marrow spaces of the skull and eventually the petrous apex, placing cranial nerves V and VI at risk.
- Posterior spread: by direct extension into the pneumatized spaces of the mastoid, where the vertical segment is at risk.
Clinical Features
Symptoms
- Penetrating, excruciating, continuous earache, out of proportion to clinical findings
- Persistent ear discharge not relieved by multiple medications (initially mucopurulent → later foul-smelling purulent and blood-tinged)
- Conductive hearing loss and sensorineural hearing loss may occur
- Facial paralysis
- Headache
- Vertigo
Signs
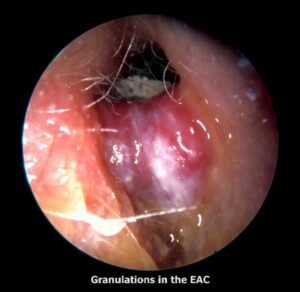
- Granulation tissue protruding into the EAC from the bony-cartilaginous junction
- Sagging of the posterior meatal wall
- Normal Tympanic membrane
- Tenderness of pinna with doughy feel on palpation
- Mastoid tenderness
- Multiple cranial nerve palsies (IX, X, XI, XII) in late stages
Investigations
- Culture sensitivity by ear swab.
- CT scan: Useful for assessing the extent of bony involvement.
- MRI: Better for evaluating soft-tissue disease, cranial nerve involvement, and can assess dural sinus patency (especially with MR angiography).
- Gallium-67 bone scan helps in confirming the diagnosis and follow-up of the patient. It is taken up by monocytes and reticuloendothelial cells, and is indicative of soft tissue infection. It can be repeated every 3 weeks to monitor the disease and response to treatment.
Differential Diagnosis
Diffuse otitis externa: Diffuse otitis externa typically shows
- Less severe pain
- Responds well to topical therapy
- Does not usually produce persistent granulation tissue with progressive cranial neuropathy
Treatment
Principles of Treatment
Treatment requires:
- Long-term anti-pseudomonal antibiotic therapy
- Daily extensive debridement of necrotic and granulation tissue
- Strict diabetic control and correction of immunocompromising factors
- Monitoring of clinical and biochemical response
Anti-pseudomonal antibiotics are required for at least 2–3 months, and prolonged therapy may be required to prevent relapse.
Effective Antibiotics
- Gentamicin combined with ticarcillin.
- Third-generation cephalosporins. e.g. ceftriaxone 1–2 g/day i.v. or ceftazidime 1–2 g/day i.v. are usually combined with an aminoglycoside.
- Quinolones (ciprofloxacin, ofloxacin and levofloxacin) are also effective and can be given orally. They can be combined with rifampin.
- Ciprofloxacin (750mg orally twice per day) seems to be the antibiotic of choice for maintainence and prolonged treatment for a minimum of 3 months to 1 year may be required, to avoid relapse.
- In case there is resistance to ciprofloxacin, antipseudomonal β-lactam agents (ceftazidime, piperacillin, imipenem) with or without combination of aminoglycoside can also be used. Aspergillus infection if found need systemic antifungal treatment.
Treatment Protocol For Malignant Otitis Externa
| Phase | Duration | Regimen |
| Induction (IV) | 2–4 weeks | Ceftazidime 2 g IV q8h + Ciprofloxacin 400 mg IV q12h |
| Step-down (Oral) | 4–8 weeks (minimum 6 weeks total) | Ciprofloxacin 750 mg PO BD |
| Total duration | Minimum 6–12 weeks | Continue until ESR/CRP normal and Gallium scan negative |
| Relapse | Extend to 6–12 months | Suspect resistance; add antipseudomonal β-lactam or imipenem |
Monitoring Parameters
Monitoring is essential to prevent relapse.
Monitoring includes
- Clinical symptoms: pain, otorrhoea, cranial nerve status
- ESR and CRP:
- weekly until normal
- then monthly
- Gallium-67 scan every 3–4 weeks
- CT/MRI only if clinical deterioration occurs
Role Of Surgery (Rare Indications)
Surgery is not routinely indicated but may be required for:
- Diagnostic biopsy to rule out malignancy
- Sequestrectomy for persistent necrotic bone not responding to antibiotics
- Drainage of abscess
Skull Base Osteomyelitis (SBO)
Definition
Skull base osteomyelitis typically occurs in an immunocompromised host with severe otalgia and unilateral otorrhoea. There may be invasion of local structures and necrosis of skin, cartilage and bone.
Cranial nerve palsies may occur due to involvement of the petrous apex, commonly affecting:
- Facial nerve (VII)
- Trigeminal nerve (V)
- Abducens nerve (VI)
- Lower cranial nerves (IX–XII)
Pseudomonas aeruginosa remains the most common organism, although other pathogens have also been identified.
Clinical Note: Chronic inflammation may cause progressive soft tissue stenosis of the EAC and result in a false fundus. This may cause conductive hearing loss, while chronic otorrhoea may cease.
Investigations
- Imaging: Cross-sectional imaging of the skull base is helpful in achieving a diagnosis and monitoring progress in SBO. High-resolution CT can demonstrate bone erosion, although magnetic resonance imaging (MRI) is more sensitive to detect skull base inflammation and cranial nerve involvement.
- Radionuclide imaging:
-
- Technetium-99m bone scan: Sensitive for bony involvement and useful for diagnosis.
- Gallium-67 scan: Used for monitoring response to treatment.
- Biopsy of any granulation tissue or sequestrum is mandatory to exclude malignancy.
- Biopsy of any granulation tissue or sequestrum is mandatory to exclude malignancy.
Management
- Fluoroquinolones (especially ciprofloxacin) are the treatment of choice and show high cure rates when used for prolonged periods.
- Hyperbaric oxygen has been used as an adjuvant therapy with some benefit, but evidence remains limited (Cochrane review found no randomised controlled trials supporting its routine use).
———— End of the chapter ————
High-Yield Points
- MOE is most commonly caused by Pseudomonas aeruginosa.
- Severe otalgia out of proportion is the most typical symptom.
- Granulation tissue at the bony-cartilaginous junction is the cardinal sign.
- MOE occurs mainly in elderly diabetics and immunocompromised patients.
- Facial nerve palsy suggests advanced MOE.
- MRI is best for soft tissue spread and cranial nerve involvement.
- HRCT is best to assess bony erosion and extent.
- Gallium-67 scan is best for monitoring response.
- ESR and CRP are the best blood markers for follow-up.
- Ciprofloxacin is the drug of choice due to bone penetration.
- Treatment requires 6–12 weeks minimum, sometimes months.
- Surgery has a limited role and is mainly used for biopsy or sequestrum removal.
- Always rule out EAC carcinoma in suspicious cases by biopsy.
NEET PG Style MCQs
- An elderly diabetic with severe otalgia and granulation tissue at bony-cartilaginous junction most likely has: A. Otomycosis B. Malignant otitis externa C. Acute otitis media D. CSOM,
- Most common organism causing malignant otitis externa is: A. Streptococcus pneumoniae B. Pseudomonas aeruginosa C. Moraxella catarrhalis D. Haemophilus influenzae,
- The most common cranial nerve involved in malignant otitis externa is: A. V B. VI C. VII D. XII,
- Best investigation for monitoring treatment response in malignant otitis externa is: A. CT temporal bone B. Pure tone audiometry C. Gallium-67 scan D. Tympanometry,
- Severe otalgia out of proportion to findings in an elderly diabetic suggests: A. Acute otitis media B. Malignant otitis externa C. Serous otitis media D. Otosclerosis,
- MRI is preferred over CT in MOE mainly because MRI is better for detecting: A. Ossicular discontinuity B. Soft tissue spread and cranial nerve involvement C. Tympanic membrane perforation D. Cholesteatoma flakes,
- A key enzyme produced by Pseudomonas that contributes to tissue invasion is: A. Hyaluronidase B. Elastase C. Coagulase D. Streptokinase,
- First-line prolonged oral antibiotic commonly used in MOE is: A. Amoxicillin B. Ciprofloxacin C. Azithromycin D. Cefixime,
- Lower cranial nerve palsies (IX–XII) in MOE suggest spread to: A. Cochlea B. Jugular foramen C. Middle ear cleft D. Eustachian tube,
- Most appropriate management of MOE includes: A. Short course topical drops only B. Mastoidectomy routinely C. Long-term anti-pseudomonal systemic antibiotics + diabetic control D. Myringotomy with grommet insertion,
Answers: 1: B. 2: B. 3: C. 4: C. 5: B. 6: B. 7: B. 8: B. 9: B. 10: C.
Clinical Case Scenarios
Case 1
A 68-year-old diabetic male has severe deep ear pain for 3 weeks, worse at night, with persistent foul otorrhoea. Otoscopy shows granulation tissue at the bony-cartilaginous junction.
Most likely diagnosis: Malignant (necrotizing) otitis externa,
Best investigation: HRCT temporal bone + MRI skull base + ESR/CRP + culture,
Best treatment: IV antipseudomonal antibiotics (ceftazidime/piperacillin-tazobactam) followed by long-term oral ciprofloxacin with strict diabetic control,
Case 2
A 72-year-old diabetic presents with MOE and now has facial deviation to the opposite side and inability to close the eye.
Most likely complication: Facial nerve palsy (CN VII involvement),
Next best step: MRI skull base + aggressive IV antibiotics, monitor ESR/CRP and Gallium scan,
Case 3
A 60-year-old immunocompromised patient has persistent otalgia and cranial nerve palsies IX and X. Otorrhoea has stopped. EAC shows narrowing and a false fundus.
Most likely diagnosis: Skull base osteomyelitis,
Best investigation: MRI skull base + Gallium scan + biopsy to rule out malignancy,
Best management: Prolonged culture-directed antipseudomonal therapy,
Case 4
A diabetic patient with suspected MOE fails to improve on ciprofloxacin. Culture shows Aspergillus species.
Most likely diagnosis: Fungal malignant otitis externa,
Best management: Systemic antifungal therapy (e.g., voriconazole) + debridement + glycemic control,
Frequently Asked Qustions in Viva
- What is the difference between malignant otitis externa and skull base osteomyelitis? Malignant otitis externa is the initial infection of the external auditory canal and temporal bone, whereas skull base osteomyelitis represents the advanced stage where infection spreads to the petrous apex, jugular foramen, and clivus, often causing multiple cranial nerve palsies.
- Why is ciprofloxacin the antibiotic of choice for malignant otitis externa? Ciprofloxacin has excellent oral bioavailability (over 80%), achieves high bone and tissue concentrations, and provides potent anti-pseudomonal activity, making it ideal for prolonged outpatient therapy after initial IV induction.
- How long should antibiotics be given for malignant otitis externa? Antibiotics should continue for a minimum of 6 weeks, but most patients require 8 to 12 weeks, and those with cranial nerve palsies or skull base osteomyelitis may need 3 to 6 months until the Gallium scan becomes negative.
- Can malignant otitis externa occur without diabetes? Yes, but it is rare and should prompt a search for other immunocompromising conditions such as HIV, hematological malignancy, chemotherapy, or long-term steroid use, and biopsy must rule out squamous cell carcinoma.
- When is surgery indicated in malignant otitis externa? Surgery is rarely indicated, but it is required for diagnostic biopsy (to rule out cancer), sequestrectomy (to remove necrotic bone), abscess drainage, and occasionally for canaloplasty to treat severe EAC stenosis after infection resolves.
- What is the cardinal sign of malignant otitis externa? The cardinal sign is granulation tissue protruding from the bony-cartilaginous junction of the external auditory canal in an elderly diabetic patient with severe otalgia that is out of proportion to clinical findings.
- Why does facial nerve palsy occur in malignant otitis externa? Facial nerve palsy occurs because the infection spreads anteriorly through the fissures of Santorini to involve the parotid gland and the facial nerve trunk at the stylomastoid foramen, or through posterior spread into the mastoid involving the vertical segment of the nerve.
- What is the role of hyperbaric oxygen in malignant otitis externa? Hyperbaric oxygen has been used as an adjuvant therapy in refractory cases, but a Cochrane review found no randomized controlled trials supporting its routine use, so it is reserved for patients who fail maximal medical and surgical therapy.
- How do you monitor treatment response in malignant otitis externa? Treatment response is monitored by serial clinical examination (pain, otorrhea, cranial nerves), weekly ESR and CRP (should trend down), and Gallium-67 scans every 3-4 weeks until negative, which indicates cure.
- What is the prognosis of malignant otitis externa? With prompt diagnosis and appropriate treatment, cure rates exceed 85%, but mortality rises to 10-20% with cranial nerve palsies and 50% with intracranial complications; relapse occurs in 15-20% due to inadequate treatment duration or poor glycemic control.
———— End ————
Download full PDF Link:
Reference Textbooks.
- Scott-Brown, Textbook of Otorhinolaryngology-Head and Neck Surgery.
- Glasscock-Shambaugh, Textbook of Surgery of the Ear.
- P L Dhingra, Textbook of Diseases of Ear, Nose and Throat.
- Hazarika P, Textbook of Ear Nose Throat And Head Neck Surgery Clinical Practical.
- Mohan Bansal, Textbook of Diseases of Ear, Nose and Throat Head and Neck Surgery
- Hans Behrbohm, Textbook of Ear, Nose, and Throat Diseases With Head and Neck Surgery.
- Salah Mansour, Middle Ear Diseases – Advances in Diagnosis and Management.
- Logan Turner, Textbook of Diseases of The Nose, Throat and Ear Head And Neck Surgery.
- Rob and smith, Textbook of Operative surgery.
- Anirban Biswas, Textbook of Clinical Audio-vestibulometry.
- Arnold, U. Ganzer, Textbook of Otorhinolaryngology, Head and Neck Surgery.
Author:

Dr. Rahul Bagla
MBBS (MAMC, Delhi) MS ENT (UCMS, Delhi)
Fellow Rhinoplasty & Facial Plastic Surgery.
Renowned Teaching Faculty
Mail: msrahulbagla@gmail.com
India
———– Follow us on social media ————
- Follow our Facebook page: https://www.facebook.com/Dr.Rahul.Bagla.UCMS
- Follow our Instagram page: https://www.instagram.com/dr.rahulbagla/
- Subscribe to our Youtube channel: https://www.youtube.com/@Drrahulbagla
- Please read. Anatomy of External Ear. https://www.entlecture.com/anatomy-of-ear/
- Please read. Anatomy of Temporal Bone. https://www.entlecture.com/anatomy-of-temporal-bone/
- Please read. Stenger’s, Chimani Moos, Teal test. https://www.entlecture.com/special-tuning-fork-tests/
Keywords: Malignant otitis externa notes, Necrotizing otitis externa MBBS, Malignant otitis externa NEET PG, Skull base osteomyelitis ENT, Malignant otitis externa symptoms, Granulation tissue bony cartilaginous junction ear canal, Pseudomonas malignant otitis externa, Malignant otitis externa ciprofloxacin duration, Gallium scan malignant otitis externa follow up, Technetium bone scan skull base osteomyelitis, HINTS differential otalgia diabetic, Facial nerve palsy malignant otitis externa, MOE vs otitis externa difference, Malignant otitis externa CT MRI findings, Skull base osteomyelitis cranial nerve palsy, MOE treatment protocol ceftazidime ciprofloxacin, Hyperbaric oxygen skull base osteomyelitis, Malignant otitis externa case presentation viva, Malignant otitis externa MCQs with answers, Necrotizing otitis externa exam guide, External auditory canal carcinoma vs malignant otitis externa, Skull base osteomyelitis ESR CRP monitoring, MOE diagnosis and management ENT, Malignant otitis externa flowchart, Malignant otitis externa mnemonics, CBME ENT malignant otitis externa,